Looking back...
Flicking through some old photos earlier this evening I found these. They were taken back in August 2007 whilst I was in A&E after multiple dislocations. The original blogs are reproduced below. The funny thing is that whilst my memory of the event is clear, the fear I felt when reading about it was something new. My main feeling if I think back to that night is how much we laughed.
First posted 19th August 2007
It happened at about 7 o'clock. We were all in the kitchen, laughing, joking, messing around, Princess Fairy Toes teasing me about my inability to cope with the three people crammed into my small kitchen, clearing up the mess from dinner, Siobhan washing up, visiting for the weekend.
I was already tired, Siobhan and I having been on a girly shopping trip earlier in the day so none too steady on my feet as I tried to open the cupboard under the sink. My hips dislocated, I wobbled and fell. As I toppled forwards the corner of the open cupboard door broke my fall before I hit the floor...unfortunately hitting smack into the corner of my collar bone and throat. The impact was hard and harsh. My collarbone popped itself out to the side, dislocating rapidly out and relocating itself back in a moment later, visibly damaging the tendon attached at the tip, running up into my neck as it went. More importantly though, my thyroid dislocated out as did my larynx.
That was it, I couldn't breathe. My throat shut firmly into spasm. Toes and Siobhan had dropped everything they were doing when I fell, Toes catching me in the small kitchen, knowing something was very wrong. He saw my collarbone pop in and out, and as I struggled to work out what had happened, my hands go to my neck, heard the crunch as I reached up and pushed my thyroid gland back into place. Later said he saw something else move around more disturbingly that he knew to be my larynx.
Both Toes and Siobhan asked if I was ok. I couldn't speak properly. I realised I couldn't really breathe either. So used are we all to falls, dislocations and any manner of trauma none of us were particularly panicked, Toes moved me into the lounge where it was lighter and more spacious so he could sit me down and see what had happened. Then he did worry. I still couldn't breathe properly. One minute I was fine, next I couldn't breathe. Couldn't speak properly to explain what was wrong. Toes wanted to know where I kept my pens. He wanted a 'biro' to hand....just in case he said. I flapped my floppy hands, wheezed a bit and managed to croak I was fine. Was breathing by then. Then I couldn't again, my throat spasmed tightly shut. Open again. Spasmed shut again. It was lasting for around a minute, minute and a half at the most. I was looking a little blue about the gills.
Toes found my ventolin inhaler and gave me a dose of that, concerned as I'm not usually wheezy. He then got the oramorph from the fridge, gave me 5mls of that which I choked and spluttered on a bit but swallowed, then promptly stopped breathing again. I'm well set up for all manner of emergencies at home, having these days an exceptional GP who prescribes wisely, but all three of us realised that this was more than typical. By now a few minutes had passed and I could speak a little, though not properly, my voice trailing off into slurring and nothingness after only a couple of words. We considered calling an ambulance, driving to A&E or staying at home and realised that I was going to have to go in, but not by ambulance. I have extremely strong views about the use of ambulances. They are for severe and life threatening emergencies only. We had access to a car, someone to drive, someone to help me, and it was probably quicker and easier just to drive. Or maybe I'm just afraid of ambulances as well as hospitals.
We found house keys and mobile phones and went out the front door. I collapsed in the road. My body was clearly struggling to cope with the shock. At my bendiest time of the month anyway, the spasms caused by multiple dislocations and shock were having huge impact sending me into what we fondly describe as a spaz attack...where I become so lax and floppy I dislocate constantly in and out of multiple joints causing me to look a bit like Elvis on a bad acid trip gone seriously, profoundly wrong. Its usually pretty amusing, especially as I tend to howl with laughter...but the lack of oxygen thing meant not so much laughing this time. That came later.
We got to the hospital quickly. Like most hospitals now you have to go through a barrier into a car park so they can later charge you to get out. A&E is no exception to this rule. Toes needed to drop us off as close as he could to A&E. It wasn't close enough. It was obvious I wasn't going to be able to walk the handful of metres to the doors. Siobhan had to half drag, half carry me into the building whilst Toes parked and ran back to get a wheelchair which he plopped me into just before I hit the floor at reception where Siobhan was struggling to hold me up.
First posted 19th August 2007
Part 2 A&E
We had to give my details at reception, name, date of birth, address, next of kin, usual stuff. All a bit difficult when you can't speak more than a croak or two and keep stopping breathing. Still a formal requirement though. Even when the details of an accident involving a cupboard door corner to the throat have been given. I made squiggly signs with my hand, but it took Siobhan to tell the receptionist that meant I wanted a pen to write down my details rather than trying to talk which by then I'd realised was making things worse.
The receptionist told us it wouldn't be long before I was seen in triage, and it wasn't. I was taken through and seen by a nurse I'd seen on a previous A&E visit. A nurse who claimed to know all about EDS. Siobhan explained to her what had happened, as I couldn't speak well enough at that point, my throat spasming too much, stopping me from breathing if I tried. Toes wandered back in towards the end of the triage assessment, he works in the same hospital. She told him she'd categorised me as yellow, so I'd be seen fairly soon, and as there was nowhere to put me in minors, I'd be safe in the waiting room as he was with me. Spending most of my life with the EDS undiagnosed and the label of attention seeking/mental has taught me a thing or two, and I knew both that she was making a bad clinical decision, and that it was personal. Whether that was directed at me or Toes I had no idea. Nor could I be bothered to do anything about it. Breathing was far more of a priority and frankly hard work.
Toes and Siobhan wheeled me back out to reception and we sat there and waited. When I was fine I was fine, but when I wasn't I really wasn't. My throat was continuing to spasm down hard every so often stopping me from breathing in. It still wasn't lasting more than a minute or two and I was getting used to it, not too worried it would carry on longer, but still a bit frightening when it was happening. Toes disappeared off a few times, looking for colleagues he might know, concerned that I'd been sent back out to sit in the waiting room.
After 20 minutes or so, the friendly looking man we'd seen coming in and out came and called me in. We'd thought he was a nurse the way he was coming out into the waiting area, and interacting with patients, but he was a senior registrar, in fact the most senior doctor in the department, and I'd noticed him keeping an eye on me earlier when I was struggling to breathe. He took us back through into the triage area, obviously none to happy with the nurses assessment and did his own. He asked me what happened, and with the help of Siobhan I managed to explain. The difference this time was that he actually did understand EDS instead of just dangerously pretending to. We managed to communicate that I'd dislocated my hip, so fallen, dislocated my collarbone and thyroid and we thought larynx too. His eyes got a bit wide when I croaked that I'd dislocated my thyroid, and he asked how I thought I might have done that. The easiest way to explain was to take his hand, place his fingers gently to my throat, and dislocate my thyroid gland back and forth. His eyes got very wide at that point and after giving me a chance to recover from the spasm that triggered off, laugh kindly at my attempts to tell him I was fine and there was nothing wrong with me I was being taken straight off to majors. I heard him very firmly telling the previous nurse that he didn't care if there wasn't any space they were to make space. If they didn't have it in 'resus' then majors would do.
The doctor wheeled me through himself and found a room in majors. A nurse came in to throw a sheet over the trolley, and that was the last contact with any nurse I had. The doctor came back in, introduced himself properly, turned on the oxygen and told me to put the mask on. He wanted to have a look in my throat, so needed me to open my mouth, at which point my jaw promptly dislocated. I gave it another go, and he managed to get a brief look. I was able to speak a bit more by this point, and so could better explain to him both what had happened and what was happening now. Mostly I tried to tell him I was fine. Nothing wrong. He seemed to find that highly amusing. He said he'd spoken to the doctor on call for ENT, and that she was already on her way in, that he expected I would need to be 'scoped' and that he was going to give me some hydrocortisone straight away. I tried to insist there was no need and my throat spasmed shut again.
The doctor went off and came back with the kit to put a drip in my arm, and the hydrocortisone injections. He chatted away to us while he put the drip in, asking about whether I was good with needles (just good at ignoring them) and joked a little about the strange position I'd naturally contorted myself into on the trolley.
By this time I'd realised that the reason my chest hurt so much was that one of my ribs was dislocated. Siobhan had let the doctor know when he came back into the room to do the drip, and after checking it, he asked if I could put it back myself. I said not a rib, but that he could. I was extremely impressed that he didn't make a fuss about unnecessary chest x-rays, and once I'd given him the go ahead, attempted a reduction there and then. The rib was determined to stay out though, so after a couple of attempts we both agreed it was best left out.
Shortly after that the on call ENT doctor arrived, surprised I think to be apologised to for wasting her time and dragging her out on a saturday night. She quickly assessed the situation, by this time a few hours had passed since I'd fallen and hit my throat, and the spasms were getting further apart, my speech much easier though my voice was exceptionally hoarse at best. She checked with Siobhan to ensure that my normal speaking voice wasn't hoarse, and I didn't usually cough the way I was, and after a quick feel of my throat/neck area and exclaiming over how incredibly lax and hypermobile it all is she decided she wanted to go ahead with the scope. She also said she'd really like to keep me in in case she had to take me to theatre, but after seeing how much I panicked at the mere mention of staying over night she said she would leave that decision until after the scope.
She went off to get the scope and prepare, and the doctor from earlier popped back in to say he was going off shift and hoped I'd be ok. We thanked him very much for all his help.
By that time I needed to go for a pee. I slid off the trolley to find I was still in full spaz attack mode. I had nothing stable in my entire body. Hips, knees, ankles, SI joint, all were flicking in and out of their sockets randomly and rapidly. Siobhan part held, part dragged me towards the toilet. To get there we had to go through the middle of two large groups of nurses, it must have been shift change. As we went to the toilet, despite being polite and lucid I was stared at with the disdain I'm sure they rightly give to vast numbers of weekend drunks, and received the same treatment on the way back...from both groups. Now, I'm used to the odd member of the public feeling that they can randomly accuse me of having been drinking if I'm flopping all over the place in say the supermarket, which is hurtful enough, but its far, far worse when 'that' look comes from supposedly highly trained professionals during an emergency medical situation. Not one of the nurses offered any help, asked if we needed a wheelchair, or in fact did anything but blatantly and openly stare.
We got back to the room just as the ENT doctor was coming back with the 'scope'. She looked at me in a totally different and perfectly acceptable way, laughed along with us, and asked if things were always this difficult for me. Talking was easier by this stage, but still hard work, so Siobhan explained things to her, including that my thyroid can dislocate, but wouldn't usually cause this kind of problem, and she very rapidly grasped that the problems were most likely being caused by the internal laxity of my throat, allowing it to fall shut on itself, spasming as a reaction to the dislocations, unlike in a non-EDS person who's collagen is nice and strong and not like melted runny chewing gum.
Whilst she was setting up her scope kit she said that ideally she'd like to keep me in for observation, even if everything was ok, but when she saw how frightened I was by this, she asked why. I told her I'd only been diagnosed with EDS for about 3 years, and before that I was 'mental'. That by now oh so familiar look flickered across her face, shock, horror, disbelief, comprehension, shame, understanding, compassion. Siobhan explained that actually although I was able to cope in hospitals as long as I thought I was going home, due to all my previous experiences staying overnight was beyond what I could cope with emotionally. I said I wasn't stupid and nor did I want to land her or the previous doctor in any hot water so if something was badly wrong on the scope then I would do as she wanted, but if it was 'just' spasming, then I wanted to go home. Please. Please.
She popped the scope in my mouth to warm it up, then into my nose and got me to swallow it down into my throat. I can think of better ways to spend a saturday night, but I've had far worse done to me. Fortunately everything was ok, nothing broken or torn inside my throat, just red, and a little swollen. The spasms were getting further apart and I was more able to cope when they did happen, so she was happy to let me go home if after a further 45 minutes without any oxygen I'd not had any problems. Siobhan was staying with me anyway, and promised to keep a close eye on me, having already chatted to the doctor earlier about handling these kind of issues, I suspect she may have agreed that in the absence of any repairable problem I'd be better off being cared for at home rather than by ward nurses rushed off their feet.
The doctor explained a little about laryngospasm, and said she was sure I'd dislocated my larynx and was now experiencing these spasms as a result of that. She was insistent that if I had any difficulty in breathing, had any noisy breathing, or got worse in any way that we were to come back in immediately.
She went went off, popping back in around 20 minutes later to check on me and give us a chance to thank her very much, then we waited another 30-45 minutes, with no further problems, and at the end of that time Toes reappeared and we started to sort ourselves out to go home.





5 comments:
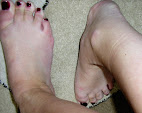
The way you're sitting in those photos: is that the way you are most comfortable. I can't sit like that because of the hip and haven't been able to for well over a decade. I also can't sit with my left leg crossed over my right one. If we could meld our two bodies we'd probably be very well off (we'll keep your figure and hair and my collagen).
Wow, what an ordeal. Glad to see you came out okay in the long run, that had to be scary.
Alhi: S'funny, cos if there was a scale for joints like there is for the autistic spectrum I think you and I would be at opposite ends waving at each other!
In the photo my position is actually restricted by the jeans I'm wearing. I'm usually more likely to have one leg tucked further over, or under the other.
The only really comfortable position for me is if I'm lying on my back (keep it clean please boys!), with my legs splayed a bit and with pillow(s) under my knees. That tips my pelvis into neutral and keeps my hips more comfy.
It does worry me that eventually I'll need new hips and that will either end up meaning I dislocate the artifical joint or that I can't learn to cope with the restricted movement.
MrN:It's on my list of accidents never to have again ;)
I thought the jeans looked as if they were holding you tight so to speak. The way you decribe is how I used to have to sleep before I got my hip replaced: I couldn't lie flat on my back without having my knees bent otherwise my back arched too much and I ended up with a sore lower back. Once the hip was replaced I remember testing it out in hospital to see if I could lie flat with my legs straight and I could!
From what you say it sounds as if you would dislocate any replacement joint and not physically be able to keep it in place so I wonder what an ortho surgeon would wish to do. It may be worth your while once the better weather comes round again to ask for a referral to one and sound them out on your hip joints just so you know your options and also if the time ever comes that a surgeon is familiar with your extreme bendyness!
Hi BG I remember reading the original post. I completely 'get' what you said about reading it through again, reading it again for me so reminded me of my recent trip to A & E it was an upsetting read for some reason second time round. Multiple dislocations are just crap crap crap - I am the same ont he sitting front - jeans help keep things in, leggings are more comfortable and I like comfortable. I sit like you. Take care
Post a Comment